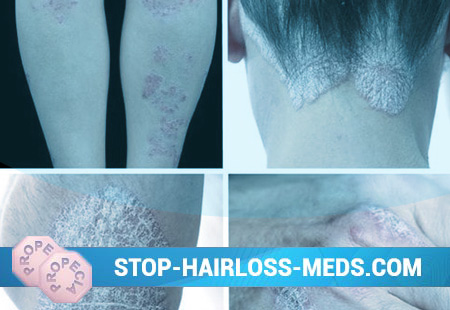
The primary elements on the skin are flat inflammatory papules. It is sharply limited, reddish-pink towering seals. Their surface is covered with dry, loosely located, easily falling silvery-white scales. The peculiar morphological structure of psoriatic papules determines the triad of symptoms pathognomonic for psoriasis, which is determined by scraping the surface of the papule with a nail or a scalpel.
Initially, due to crushing of flakes, a pattern is observed that resembles that when scraping a frozen drop of stearin, a sign of a stearic stain. Then, due to the fact that between the prickly and horny layers there is no granular layer connecting them, the compact layers of the horny plates are separated in the form of a film, exposing the wet surface of the spinous layer (a sign of a psoriatic film). Further slight scraping leads to damage to the capillaries in the elongated papillae, with the release of droplets of blood (a symptom of blood dew, a symptom of point bleeding).
The lesion begins with a rash of miliary papules, which, gradually increasing along the periphery, turn into lenticular and nummular, merge with each other and form a different-sized plaque. In the development of the psoriatic process on the skin, three stages can be identified.
The first stage is progressive, which is caused by the appearance of new papules on the skin and an increase in the size of existing elements with the formation of an erythematous border around the lesions, which is called a peripheral growth zone. The marginal zone of the plaque is free from peeling. It, being the final stage of the inflammatory process, as if not keeping pace with the growth of psoriatic elements.
In the acute phase of psoriasis, the formation of psoriatic papules can occur on the spot, even minor trauma to the skin (Kebner symptom) – with sunburn, rubbing irritating ointments, injection with an injection needle, scratches, etc. skin, in stressful situations. So psoriatic erythroderma is formed. Over time, the development of new papules and peripheral growth of elements is completed, the peeling can increase up to the defeat of the entire surface of the skin or mucous membrane, and psoriasis flows in the stationary period.
In this stage, the emergence of new elements ceases, but the size of existing papules and plaques remain unchanged. Education papules can end at any stage. Therefore, in the stationary period, both nummular and lenticular and even miliary papules can be seen simultaneously. Often there is a common rash, papules can be lenticular in size, and this is where the development of the process stops. This course of psoriasis is usually determined by local infection in the tonsils (tonsillogenic psoriasis). In the stationary period, after cessation of papule growth, a gentle folding of the stratum corneum 2–7 mm wide is often formed around it. After resorption of psoriatic lesions, temporary hypopigmentation (leucoderma or a lighter skin area) appears, less often – hyperpigmentation (darker skin area).
The third stage is regressive (reverse), one of the main signs of which is the gradual disappearance of lesions with the appearance of a pseudosclerotic whitish rim (Voronov’s rim) around the lesions. Only a small number of patients have a slight itch. Subjective feelings are mild or may be absent altogether. The resolution of psoriatic elements is carried out in their central part.
Semicircular shapes appear, which are characteristic of the progressive period of psoriasis. It is also taken into account that the central resolution of psoriatic plaques may be accompanied by their peripheral growth. In such cases, determine the diagnosis of progressive psoriasis. The different mutual arrangement of psoriatic elements of various sizes, their peripheral growth and resolution in the center lead to the formation of extensive foci of garland-like outlines, which at times resemble a geographical map. Rashes can occur anywhere on the skin, but mostly located on the extensor surfaces of the limbs, especially the knee and elbow joints, in the sacrum, and scalp, especially on the edge of hair growth (“psoriatic crown”). The structure of hair in psoriasis does not change, and the hair does not fall out.
On the extensor surface of the elbow and knee joints, plaques are very often saved for an indefinitely long period of time after the resolution of the rest of the rash (the so-called “duty” plaques). In some patients, there is a lesion of the skin folds (axillary, under the mammary glands, inguinal-femoral), and often it can be isolated. In the latter, due to increased humidity, there is no flaking, and the lesions resemble infectious (for example, streptococcal or candidal) diaper rash. The clinical signs of psoriasis are manifested by severe infiltration, the absence of a horn corolla along the peripheral surface of the plaque and the ability to detect two symptoms of the psoriatic triad – the psoriatic film and blood dew.
One of the features of the rash is symmetry and prevalence (this is typical for the clinic of vulgar psoriasis). Sometimes, as a result of a pronounced, progressive course of the process, in the absence of a resolution, a continuous lesion of the skin of large areas of the body (diffuse psoriasis) and even of the entire skin (universal psoriasis) is formed. In rare cases, the elements of the rash are located on a limited area of the skin (scalp, penis) stripes, asymmetrically, on one half of the body. Psoriasis in children is recognized by the appearance of not nodules, but erythematous foci, most often in the folds of the skin. Sharply outlined pink-red areas tend to peel off. But at times, when the exudation characteristic of children is manifested, maceration and detachment of the horny layer along the periphery can be observed, which may be similar to diaper rash. In children, rash appears in places not typical for psoriasis (face, natural folds, genitals). Often, the first rash forms on the scalp, where, against the background of a slightly infiltrated erythema, clusters of crusty scales form. The most common rashes are located on the red border of the lips, the mucous membrane of the cheeks, tongue. Clinic of lesions of the oral mucosa in psoriasis depends directly on the form of the disease. If a psoriatic plaque forms at the bottom of the oral cavity, then the lesion may be irregular in outline, its surface looks like a sticky film. There is always an inflammatory corolla around such a hearth. In very rare cases, a burning sensation may be associated with psoriatic lesions. Rashes in the mouth are expressed during the exacerbation of the psoriatic process on the skin, however, rashes on the mucous membrane of the mouth disappear and the skin is not always a lump sum. In pustular psoriasis, the mucous membrane is drawn into the process much more often than in normal form. It affects mainly language. In addition to the described classical picture of psoriasis, there are its various variants and quite special forms of the course of the disease in the form of arthritis and erythroderma. Pustular psoriasis is manifested by purulent elements of a superficial nature. There are pustular psoriasis disseminated (type Zumbusha) and palms and soles (type Barber).
Irritated psoriasis. As a result of interaction on the skin of patients with progressive psoriasis, sun rays, irritating ointments, or any other irritants, the plaques become cherry-red in color, become more convex, and a wide hyperthemic belt appears around them, which lubricates the sharpness of the boundaries (after the plaque resolves, it becomes wrinkled ).
Spotted psoriasis. It is manifested by mild infiltration of elements of the rash, which are seen not as papules, but as spots. Formed usually sharp and similar to toksidermiya. The most important differential diagnostic technique is the identification of the psoriatic triad.
Seborrheic psoriasis. Manifested in patients with seborrhea. On the scalp, as well as behind the auricles in the nasolabial folds, on the chest, scapular and subscapular areas of the back, psoriatic scales are saturated with sebum, stick together, stick to the surface of plaques, simulating a picture of seborrheic eczema.
Old psoriasis. This form of the disease can be described by pronounced infiltration of plaques, their bluish color, warty and hyperkeratotic surface. Such foci of psoriasis with great difficulty are treated, and sometimes, extremely rarely, are transformed into a malignant tumor.
Exudative psoriasis. This form of the disease is represented by an excessively pronounced exudative component of the inflammatory response in the progressive period of the disease. Exudate, making its way to the surface of the papule, saturates the accumulation of scales, turning them into formations similar in appearance to the crusts. These secondary elements of the skin rash are called flaky crusts, while having a yellowish color. After their removal, a weeping, slightly bleeding surface is exposed. Drying and layering on each other, scale-crusts can form a dense massive conglomerate, similar to an oyster shell (rupioid psoriasis).
Palmar and plantar psoriasis. It can be detected either by ordinary psoriatic papules and plaques, or by hyperkeratotic, simulating corns and callousness. Sometimes there is a continuous damage to the surface of the skin of the palms or soles in the form of increased keratinization, thickening.
The boundaries of such a lesion are distinct (a characteristic feature of psoriatic plaques). In other rare cases, the palmar and plantar psoriasis may be limited to coarse-shaped peeling.
Psoriasis of the nails. There are three forms of nail damage: atrophic, pinpoint, hypertrophic onycho-dystrophy. A point lesion is described as the formation of pinholes in the nail plates that resemble a working surface of a thimble. Another manifestation of nail psoriasis is extremely similar to onychomycosis: the nail plate from the free edge is modified in color, characterized as dull, easily crumbled. A sign that in these cases can distinguish psoriasis from onychomycosis is an inflammatory rim around the periphery of the affected part of the nail, which is the edge of the papule in the nail bed, translucent through the nail plate. In the atrophic form of onychodystrophy, thinning of the substance of the nail without prior inflammatory changes becomes noticeable. The nail plate gradually becomes significantly thinner, separates from the nail bed, gradually disappears, leaving a small gray residue at the hole. Psoriasis of the mucous membranes is extremely rare. In normal psoriasis, the mucous membrane of the mouth is seized in 2% of patients, most often the rash is located on the tongue, cheeks, lips. Irregular oval shapes appear, bulging above the surrounding mucosa, sharply delimited nodules of a grayish-white color with a pink rim around. At an established stage of its development, the rash can be covered with a whitish, loose patina, which can be easily removed with a spatula. After the removal of such a plaque, a bright red surface is exposed with signs of point or parenchymal hemorrhage.
Psoriatic arthritis. In some patients with psoriasis due to infiltration of periarticular tissues, a lesion of the joints occurs (arthropathic psoriasis). The predominantly interphalangeal joints are affected, but large joints can also be drawn into the pathological process and, very rarely, the sacroiliac joints and the joints of the spine. Initially, patients complain only of pain in the joints (arthralgia), then their swelling is formed, movements are limited, subluxations and dislocations can occur. On radiographs, osteoporosis and narrowing of the joint space are visible.
The process can end with ankylosis and persistent deformities of the joints, which leads to disability. It must be remembered that, unlike other arthritis (inflammation of the joints), psoriatic arthritis is formed in the presence of psoriatic rash, which can often be accompanied by damage to the nails, and also that its onset coincides with the exacerbation of the skin process, which usually acquires nature of exudative psoriasis.
Psoriatic erythroderma. In some patients with psoriasis, most often in the progressive period under the pressure of various irritating factors (autointoxication, vigorous rubbing of the skin with a washcloth, solar irradiation, hot baths, irrational treatment), body temperature can suddenly increase and erythema (red rashes) develop. Initially, they are formed on psoriatic rash-free areas of the skin, then they are combined into continuous erythroderma. Papules and plaques are indistinguishable. The affected skin flakes off strongly with thin lamellar scales; Often hair falls out, nails thicken and easily exfoliate. After a few weeks, erythroderma ends and the usual pattern of psoriasis is restored. In most patients, the disease is characterized by seasonality.
Relapses occur in the autumn-winter (winter form) and spring-summer (summer form) periods. This fact must be known when prescribing a course of treatment, including a sanatorium.
