What is Dermatomyositis (Polymyositis)?
Dermatomyositis (polymyositis) is a systemic disease with a predominant lesion of the skin and muscles, as well as various changes in the internal organs. The disease has several more names: polymyositis, poikilodermatomyositis, sclerodermatomyositis, angiomyositis, generalized myositis, generalized fibromyositis.
Causes of Dermatomyositis (Polymyositis)
Dermatomyositis (polymyositis) can cause hypothermia, prolonged exposure to the sun, vaccinations, pregnancy, various drugs, injuries, and viral infections. In some patients, a connection has been established between dermatomyositis and a cancerous tumor, i.e., a cancerous tumor can cause dermatomyositis.
Pathogenesis during Dermatomyositis (Polymyositis)
In the pathogenesis of dermatomyositis, the leading role is played by autoimmune processes, as a result of which auto-antibodies to muscles are formed, immunoglobulins are deposited in the vessels of skeletal muscles. In addition to the autoimmune mechanism, the cause of dermatomyositis can be the neuroendocrine reactivity of the body at certain periods of life. The disease can develop in transitional ages (adolescent and menopause).
Symptoms of Dermatomyositis (Polymyositis)
Dermatomyositis (polymyositis) can begin either acutely or develop gradually. A characteristic manifestation of the disease is muscle syndrome in the form of muscle weakness, muscle pain. The body temperature rises to very high values, pains in the joints, dense common swelling, and skin lesions appear. In all patients, skeletal muscles are affected. Muscle pains arise not only with movements, but also at rest, with pressure on them. Muscle weakness is characteristic. The muscles themselves increase in volume and become denser. As a result of weakness in the muscles, active movements are disturbed, patients can not raise their limbs, sit on their own. Dermatomyositis is characterized by damage to the muscles of the neck and shoulder girdle, due to which the movements of the head are disturbed, up to the inability to keep it sitting or standing. In the case of the prevalence of the process, patients are essentially completely immobilized, and in especially severe cases, a state of complete prostration develops. If the pathological process develops in the facial muscles, then the face becomes masked, damage to the pharyngeal muscles leads to a violation or inability to swallow. Damage to breathing is caused by damage to the intercostal muscles and diaphragm. The oculomotor muscles can be affected, which leads to the corresponding symptoms of the organ of vision. Dermatomyositis must be distinguished from neurological symptoms in true lesions of the nervous system.
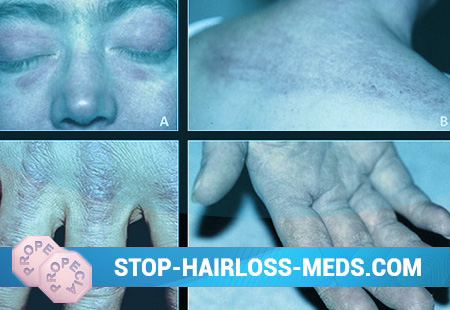
In the early stages of the disease, swelling and muscle soreness are noted. Later, muscle fibers become dystrophic, up to resorption, followed by replacement of the fibers with connective tissue, i.e., myofibrosis develops. Muscles atrophy, contractures appear. Less commonly, calcium is deposited in the muscles. Calcification also develops in the subcutaneous tissue, especially in patients of a young age. With dermatomyositis, skin lesions are very diverse. These are mainly erythema in the open parts of the body, as well as papular, bullous (vesicular) rashes, purpura, spider veins, areas of keratinization of the skin, increased or decreased pigmentation, up to the disappearance of pigmentation in certain areas of the skin. Often the rash is accompanied by itching. A very characteristic skin manifestation of the disease is the presence of edema around the eyes with purplish-purple erythema, the so-called dermatomyositis glasses.
With dermatomyositis (polymyositis), internal organs are affected. The cardiovascular system is characterized by myocarditis (inflammation of the heart muscle) or myocardial dystrophy. Myocardial lesions lead to tachycardia (palpitations) and heart rate inconsistency, low blood pressure, expansion of the heart to the left, systolic murmur at the apex, etc. With widespread myocardial damage, heart failure develops. The lungs are affected either due to a pathological process in the intercostal muscles or diaphragm, or as a result of a secondary infection. This is due to the predisposition of patients to bacterial infections due to hypoventilation (decreased ventilation) of the lungs or a violation of swallowing and aspiration of food. In the acute course of patients, shortness of breath, often significant, is concerned, and cyanosis of the skin (cyanosis) develops. Possible slowly developing pulmonary fibrosis with the development of hypertension in the pulmonary circulation and pulmonary heart.
Almost half of the patients have gastrointestinal pathologies. They are manifested by a lack of appetite, abdominal pain, inflammatory reactions from the stomach and small intestine. Due to developing muscle pathology, hypotension of the upper third of the esophagus is characteristic, the mucous membranes of the stomach and intestines with edema, hemorrhages, up to the formation of necrosis, can be affected. There may be severe gastrointestinal bleeding, perforation of the stomach and intestines, and sometimes intestinal intolerance. At the height of the disease, diffuse glomerulonephritis or mild albuminuria usually develops. Half of patients have enlarged liver and spleen, lymph nodes in various parts of the body.
The course of the disease is acute, subacute and chronic. The acute course is characterized by an extremely rapid increase in damage to the striated muscles, up to complete immobility, impaired swallowing and speech. Often there is a severe picture of a toxic disease with high fever, a variety of skin rashes. If untreated, after 3-6 months, death can occur due to aspiration pneumonia, pulmonary heart disease due to severe damage to the heart and lungs.
In the subacute course, the disease has a cyclical nature, but the pathological process in this case is steadily progressing with an increase in weakness, damage to the skin and internal organs. In this course of the disease, there can also be a fatal outcome, but with adequate treatment, it is possible to recover or go into a chronic course with the development of contractures, calcifications, and impaired motor activity of patients.
The most favorable form of dermatomyositis is a chronic form, which also has a cyclic course. Only individual muscles are affected. The condition of patients remains satisfactory for a long time, working capacity remains. Among this category of patients there are exceptions. These are patients who develop extensive calcifications (deposits of calcium salts) in the skin and subcutaneous tissue, as well as in the muscles, which leads to persistent contractures and immobility.
Diagnosis of Dermatomyositis (Polymyositis)
The diagnosis of dermatomyositis is made on the basis of clinical manifestations, electromyographic data (studies of the electrical activity of muscles) and laboratory data. Leukocytosis is usually observed in the blood, usually moderate, in the leukocyte formula – pronounced eosinophilia (up to 25-70%), iron deficiency anemia (anemia) is rarely detected. In the acute course, moderately but persistently accelerated ESR (erythrocyte sedimentation rate).
A characteristic is considered to be an increase in the activity of enzymes: aldolases, lactate dehydrogenase, creatine phosphokinase, aspartate and alanine notransferases. Creatinuria (an increase in urine cretinin) is very important. Microscopic examination of striated muscles taken by biopsy shows a thickening of muscle fibers with loss of transverse striation, impaired trophism, up to necrosis.
Treatment of Dermatomyositis (Polymyositis)
With all forms of the course of dermatomyositis, treatment with corticosteroid hormones (glucocorticoids) is indicated. The use of steroid hormones changes the course and poor prognosis of the disease. Large daily doses of hormones are recommended: prednisone – 60-80 mg, dexamethasone – 6-8 mg for 2-3 months, sometimes more.
After achieving the therapeutic effect, the dose of hormones is reduced very slowly (per tablet every 7-10 days) to a maintenance dose against the background of delagil (0.25 g), plaquenil (0.2 g), one tablet in the evening. Only with persistent remission can hormones be completely canceled. Triamnupolon is contraindicated because of the ability to increase muscle weakness. During treatment with glucocorticoids, inflammatory seals in the skin and muscles disappear, swallowing normalizes, speech, the cardiovascular system returns to normal. But the improvement comes very slowly: first, the function of smooth muscles improves, then – striated.
Pyrazolone series preparations are used in usual doses. In chronic focal infections (tonsillitis, sinusitis), antibiotics are prescribed. In complex treatment, vitamins for injection are recommended: vitamin B1 (30-40 injections), B6 (10 injections per course every other day), B12 (20 injections of 200 micrograms every other day), intravenous vitamin C. Inside vitamin B2 (30-40 days ) To improve muscle function, proserin, ATP, cocar-boxylase, nerobol are used. In the presence of calcifications, the disodium salt of ethylenediaminetetraacetic acid (Na2 ED -TA) is used intravenously in a 5% glucose solution. The course is 3-6 days, 7 days off and repeat again. With damage to the kidneys and liver, the drug is contraindicated. When removing the severity of the process, careful therapeutic exercises, massage of the limbs are shown.
Forecast
The prognosis is satisfactory, especially in young people. With early treatment with adequate doses of hormones, a lasting recovery occurs. In the chronic course, an undulation of the clinical manifestations of the disease is observed.
Prevention of Dermatomyositis (Polymyositis)
Specific (primary) prevention of dermatomyositis (polymyositis) has not been developed. Secondary is the follow-up, supportive treatment with corticosteroids, sanitation of foci of chronic infection, reduction of allergization of the body.